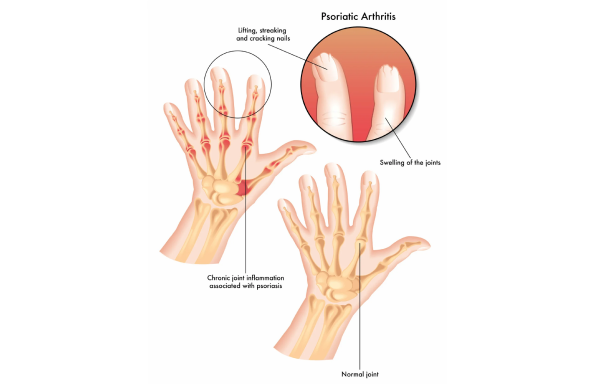
Causes of Psoriatic Arthritis
The exact cause of PsA is unknown, but it involves a combination of genetic, immune, and environmental factors:
- Genetic predisposition: Family history of psoriasis or PsA
- Immune system dysfunction: Abnormal immune response attacking healthy cells
- Environmental triggers: Infections, injuries, or stress
Symptoms of Psoriatic Arthritis
Symptoms can vary but commonly include:
- Psoriasis Rash: silver-gray scaly patches on skin
- Joint pain and stiffness
- Swollen fingers and toes (dactylitis).
- Fatigue
- Nail changes such as pitting, thickening, or separation from the nail bed.
Associated Conditions
Psoriatic arthritis is often associated with several other conditions, including:
- Psoriasis: A chronic skin condition characterized by red, scaly patches.
- Uveitis: Inflammation of the eye, which can lead to redness, pain, and vision issues.
- Cardiovascular disease: Increased risk of heart disease and related conditions.
- Metabolic syndrome: A cluster of conditions including high blood pressure, high blood sugar, and abnormal cholesterol levels.
Prognosis of Psoriatic Arthritis
PsA is a chronic condition with periods of flare-ups and remission. Early diagnosis and treatment can help manage symptoms and prevent joint damage. The prognosis varies, but with proper management, many people lead active lives.
Diagnosis of Psoriatic Arthritis
Diagnosis involves:
- Medical history and physical examination
- Imaging tests such as X-rays, MRI, CT scan, or ultrasound
- Blood tests to rule out infection (complete blood count), check for other types of arthritis, and look for inflammatory markers (erythrocyte sedimentation rate, C-reactive protein)
Pain Medicine Intervention for Psoriatic Arthritis
PsA can usually be treated with pain medicine intervention, activity modification, and conservative treatment options. These include:
- NSAIDs: Nonsteroidal anti-inflammatory drugs like ibuprofen or naproxen to reduce pain and inflammation.
- DMARDs: Disease-modifying antirheumatic drugs to slow disease progression.
- Biologic agents: Target specific parts of the immune system to reduce inflammation.
- Corticosteroids: Oral or injectable steroids to control severe inflammation and pain.
- Topical treatments: Creams and ointments to reduce pain and inflammation in affected joints.
- Physical Therapy
Treatment of Psoriatic Arthritis
Treatment aims to control inflammation, relieve pain, and improve joint function:
- Medications such as NSAIDs, DMARDs, biologics, and corticosteroids.
- Physical therapy to maintain joint flexibility and strength.
- Lifestyle changes including exercise, stress management, and healthy diet.
- In severe cases, surgery may be needed to repair or replace damaged joints.
Treatment Videos
Lifestyle
References
- Cleveland Clinic. (19 September 2023). Psoriatic arthritis. https://my.clevelandclinic.org/health/diseases/13286-psoriatic-arthritis
- Johns Hopkins Medicine. (n.d.) Psoriatic arthritis. (n.d.). https://www.hopkinsmedicine.org/health/conditions-and-diseases/psoriatic-arthritis
- Mayo Clinic Staff. (02 October 2021). Psoriatic arthritis. (n.d.). https://www.mayoclinic.org/diseases-conditions/psoriatic-arthritis/symptoms-causes/syc-20354076
- National Psoriasis Foundation. (n.d.) Psoriatic arthritis. https://www.psoriasis.org/about-psoriatic-arthritis/
- NHS. (06 September 2023). Psoriatic arthritis. https://www.nhs.uk/conditions/psoriatic-arthritis/
- Radiopaedia. (n.d.). Psoriatic arthritis of the hands. https://radiopaedia.org/cases/psoriatic-arthritis-of-hands